Why are under 30s being offered a different Covid vaccine? Rare AstraZeneca blood clot side effect explained
and live on Freeview channel 276
People under the age of 30 will be offered an alternative to the AstraZeneca Covid-19 vaccine, due to concerns over a possible link between “extremely rare” blood clots.
The Medicines and Healthcare products Regulatory Agency (MHRA) has not concluded that the vaccine causes rare brain clots, but after 79 reported cases in the UK, the regulator says the link is now getting stronger.
Advertisement
Hide AdAdvertisement
Hide AdBut why has the vaccine been stopped for only young adults? Here’s what you need to know.
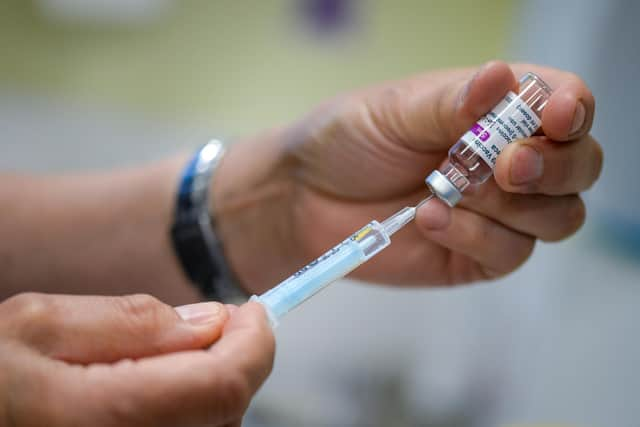

Why has AstraZeneca been stopped for under 30s?
Young adults aged between 18 and 29 will be offered the Pfizer or Moderna vaccine, or another Covid-19 jab that becomes available on the UK’s vaccination programme.
The decision to stop administering the AstraZeneca vaccine to this age group comes after the MHRA said the balance of risk for the jab is very favourable for older people, but is “more finely balanced” among younger groups, who do not tend to suffer serious illness from coronavirus.
Professor Wei Shen, chairman of the Joint Committee on Vaccination and Immunisation (JCVI), said the recommendation to give other vaccines to AstraZeneca for the under-30s was “out of the utmost caution”, rather than because of “any serious safety concerns”.
Advertisement
Hide AdAdvertisement
Hide AdDr June Raine, chief executive of the MHRA, told a briefing that the clots were “extremely rare”, adding that the benefits of the vaccine still outweigh the risks.
She said: “Based on the current evidence, the benefits of the Covid-19 vaccine AstraZeneca against Covid-19 and its associated risks – hospitalisation and death – continues to outweigh the risks for the vast majority of people.
“Our review has reinforced that the risk of this rare suspected side effect remains extremely small.”
But she added: “The evidence is firming up and our review has concluded that while it’s a strong possibility, more work is needed to establish beyond all doubt that the vaccine has caused these side effects.”
Advertisement
Hide AdAdvertisement
Hide AdProfessor Sir Munir Pirmohamed, chairman of the Commission on Human Medicines, added that any risks from the vaccine had to be set against the fact around 30 per cent of people with Covid suffer low blood platelet counts, while the virus also “causes clotting”.
Some 7.8 per cent of people with Covid suffer blood clots on the lungs, while 11.2 per cent will suffer deep vein thrombosis (DVT).
He said there appears to be a “slightly higher risk in the younger age group” of clots after the AstraZeneca vaccine, but the reason is “not clear” with further work required.
On possible explanations for the clots, he said: “The early evidence suggests that this constellation of symptoms is caused by an immune response against platelets which allows the platelets to then lead to clotting in different parts of the body.
Advertisement
Hide AdAdvertisement
Hide Ad“But what we don’t have clearly is the link between the vaccine and how the immune response becomes activated against the platelets.”
How many cases of blood clots have there been?
Up to 31 March, the MHRA in the UK has received 79 reports of blood clots accompanied by low blood platelet count.
These cases all occurred in people who had their first dose of the vaccine, out of around 20 million doses given.
Of these 79, a total of 19 people have died, although it has not been established what the cause was in every case.
Advertisement
Hide AdAdvertisement
Hide AdThe 79 cases occurred in 51 women and 28 men, aged from 18 to 79. Of the 19 who died, three were under the age of 30, the MHRA said.
Some 14 cases of the 19 were cerebral venous sinus thrombosis (CVST), a specific type of clot that prevents blood from draining from the brain. The other five cases were other kinds of thrombosis in major veins.
The figures suggest the risk of rare blood clot is the equivalent to four people out of every million who receive the vaccine.
Separately, a review by the European Medicines Agency (EMA) concluded on Wednesday (7 April) that “unusual blood clots with low blood platelets should be listed as very rare side effects” of the Oxford/AstraZeneca vaccine.
Advertisement
Hide AdAdvertisement
Hide AdThe EMA has carried out an in-depth review of 62 cases of CVST and 24 cases of splanchnic vein thrombosis in which 18 people died.
Andrew Pollard, professor of paediatric infection and immunity, and lead investigator of the Oxford University trial of the vaccine, said safety had been a “priority” throughout its development last year.
He said: “We are reassured to see that safety monitoring continues under the close scrutiny of regulators and public health authorities as the vaccine is rolled out around the world.
“The identification of rare cases of blood clots, which might be associated with the vaccine, shows that the safety system works, and has also allowed MHRA and EMA to conclude that the benefits of vaccination continue to outweigh the risks, while putting in measures to help mitigate any possible risk.”
Should I still get my second dose?
Advertisement
Hide AdAdvertisement
Hide AdThe MHRA has said that those who have had their first dose of the AstraZeneca vaccine should still get their second dose, and only those who suffered a rare blood clot after the first dose should not get vaccinated.
Anyone with blood disorders that leave them at risk of clotting should discuss the benefits and risks of vaccination with their doctor before going for a jab.