Wegovy: ‘game changer’ weight loss jab used by celebrities to be made available on NHS
and live on Freeview channel 276
A “game changer” weight loss injection said to be popular among celebrities is to be made available through the NHS.
Thousands of people living with obesity in England are expected to be offered the appetite suppressant Wegovy on prescription after the National Institute for Health and Care Excellence (Nice) approved its use.
Advertisement
Hide AdAdvertisement
Hide AdThe decision has been described by health experts as a “pivotal moment” for the treatment of people living with obesity, but others warned the drug is not a “quick fix”.
Wegovy, also known as semaglutide, has been used by the likes of Billionaire Elon Musk to keep in shape. Last October, Musk was asked by a Twitter user what his secret was to looking "fit, ripped, and healthy" to which he replied "fasting" and "Wegovy".
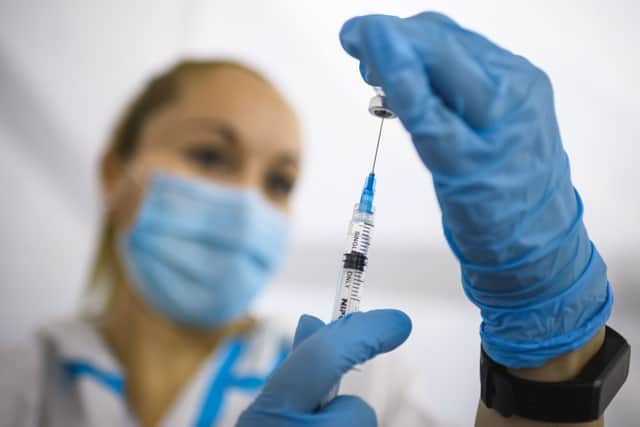

A previous study found that people who are given the drug, which comes as a weekly injection, saw their weight drop by 12% on average after 68 weeks.
Nice has issued final guidance recommending semaglutide, which is made by Novo Nordisk, for adults with at least one weight-related condition and a body mass index (BMI) score of at least 35.
Advertisement
Hide AdAdvertisement
Hide AdThe weight-related conditions that make obese people eligible for the drug include:
- type 2 diabetes
- prediabetes
- high blood pressure
- dyslipidaemia (unbalanced or unhealthy cholesterol levels)
- obstructive sleep apnoea
- heart disease
In some cases, people with a BMI of 30 and over may be able to access the drug, which is given via a pen injector.
People will only be given Wegovy on prescription as part of a specialist weight management service involving input from several professionals, and for a maximum of two years. The drug is to be used alongside a reduced-calorie diet and increased physical activity, Nice said.
Patients inject themselves with the drug weekly, which suppresses the appetite through mimicking the hormone glucagon-like peptide-1 (GLP-1) that is released after eating. This makes people feel full, meaning they eat less and lose weight.
Advertisement
Hide AdAdvertisement
Hide AdA previous study, published in the New England Journal of Medicine, found that nausea and diarrhoea were the most common side effects but these were “typically transient and mild-to-moderate in severity and subsided with time”.
Helen Knight, director of medicines evaluation at Nice, said: “For some people losing weight is a real challenge which is why a medicine like semaglutide is a welcome option. It won’t be available to everyone.
“Our committee has made specific recommendations to ensure it remains value for money for the taxpayer, and it can only be used for a maximum of two years. We are pleased to finally publish our final guidance on semaglutide which will mean some people will be able to access this much talked about drug on the NHS.”
Prof Nick Finer, honorary clinical professor at the National Centre for Cardiovascular Prevention and Outcomes at UCL, added: “The efficacy of semaglutide is a true game changer for the medical treatment of obesity, a chronic disease that shortens life through its many complications.”
Advertisement
Hide AdAdvertisement
Hide AdMeanwhile, Charity Beat raised concerns about the impact of the drug on people with eating disorders. Tom Quinn, Beat’s director of external affairs, said: “Weight-loss medications like semaglutide can be extremely attractive to people with eating disorders as they appear to provide quick results.
“However, these medications can be very dangerous as they can worsen harmful thoughts and behaviours for those unwell, or contribute to an eating disorder developing for someone who is already vulnerable.”
The drug will be available to NHS patients soon when the launch of the drug in England is confirmed by manufacturer Novo Nordisk. The NHS in England is required to implement the Nice recommendations within three months of the product becoming commercially available.
In February it emerged that some high street chemists in England will prescribe the drug, if suitable, through their online doctor services.
Advertisement
Hide AdAdvertisement
Hide AdA spokesperson for Novo Nordisk said: “Novo Nordisk welcomes the final Nice recommendation for Wegovy (once-weekly semaglutide 2.4mg), as an option for weight management within the NHS. We are working to make Wegovy available in the UK as soon as possible.”
Comment Guidelines
National World encourages reader discussion on our stories. User feedback, insights and back-and-forth exchanges add a rich layer of context to reporting. Please review our Community Guidelines before commenting.
