'As likely as being hit by a plane in your home' - odds of developing a deadly blood clot from AstraZeneca vaccine less than 0.0001%
and live on Freeview channel 276
Young adults under the age of 30 will be offered an alternative to the AstraZeneca Covid-19 vaccine, as investigations continue into the potential link with blood clots.
While the Medicines and Healthcare products Regulatory Agency (MHRA) has not concluded that the “extremely rare” blood clots in the brain are caused by the vaccine, the regulator has said that the link is getting stronger.
Advertisement
Hide AdAdvertisement
Hide AdAs such, people aged between 18 and 29 will instead be offered the Pfizer or Moderna vaccine, or another Covid-19 jab that becomes available in the UK.
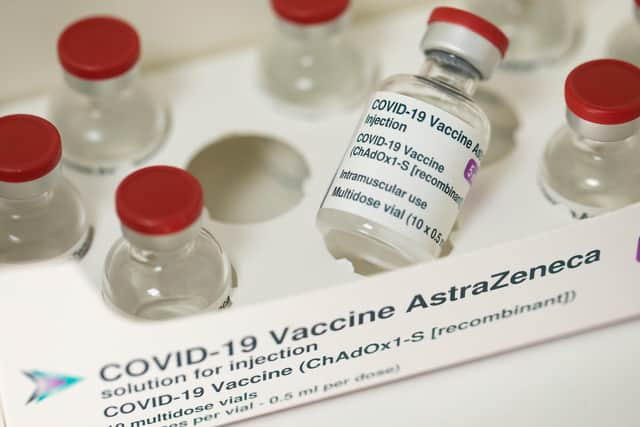

But how common are blood clots after getting the AstraZeneca vaccine, and what are the odds of clots developing? Here’s what you need to know.
How many cases of blood clots have been reported?
A total of 79 cases of blood clots accompanied by low blood platelet count have been reported in the UK up to 31 March, according to the MHRA.
In all of these cases, the blood clots occurred in people who had received their first vaccine dose, out of around 20 million doses given.
Advertisement
Hide AdAdvertisement
Hide AdA total of 19 people from these 79 later died, although it has not been confirmed what the cause of death was in every case.
Blood clots occurred in 51 women and 28 men, aged from 18 to 79, and of the 19 who died, three of these were under the age of 30.
Some 14 cases of the 19 were cerebral venous sinus thrombosis (CVST), a specific type of clot that prevents blood from draining from the brain, while the other five were other kinds of thrombosis in major veins.
The decision to stop administering the AstraZeneca vaccine to this age group comes after the MHRA said the balance of risk for the jab is very favourable for older people, but is “more finely balanced” among younger groups, who do not tend to suffer serious illness from coronavirus.
What are the odds of developing a blood clot from the vaccine?
Advertisement
Hide AdAdvertisement
Hide AdProfessor Sir Munir Pirmohamed, chairman of the Commission on Human Medicines, said that any risks from the vaccine had to be set against the fact that around 30 per cent of people with Covid suffer low blood platelet counts, while the virus also “causes clotting”.
Some 7.8 per cent of people with Covid suffer blood clots on the lungs, while 11.2 per cent will suffer deep vein thrombosis (DVT).
As only 79 cases of blood clots, and 19 deaths, have been reported after 20 million vaccine doses, the risk of dying after receiving the AstraZeneca jab is only 0.000095 per cent.
The figures from MHRA suggest the risk of developing a rare blood clot is the equivalent to four in every 1,000,0000 who receive the vaccine.
Advertisement
Hide AdAdvertisement
Hide AdHowever, if you choose not to get the vaccine and you later catch Covid-19, you are two per cent more likely to develop a blood clot, with around 3,000 people per month in the UK suffering from them.
To put the figures in perspective, around two in every 1,000 women are likely to develop a blood clot during or after pregnancy, while women who take the contraceptive pill have a one in 2,000 chance of getting a blood clot.
These reports have deterred many young women from taking the pill, even though the risk of taking it is about the same as being struck by lightning - which has little more than a one in 10,000 chance.
Getting the flu jab poses a one in one million risk of developing Guillain-Barré syndrome, a rare disease that can leave you paralysed. However, this is about the same level of risk as dying in an accident while on a 10 mile bicycle ride.
Advertisement
Hide AdAdvertisement
Hide AdResearch from BMJ Best Practice shows that the risk of developing a blood clot from the vaccine is lower than being hit by an aeroplane in your own home, which has a one in 250,000 chance.
Around three to five per cent of people travelling by plane also run the risk of suffering with a blood clot.
The BMJ defines risks with a 0.0001 percentage risk, or one in 100,000 to one in 1,000,000, as ‘minimal’.
As the risk of dying from Covid-19 after the vaccine is 0.000095 per cent, this is even lower than what is defined as a minimal risk.
Advertisement
Hide AdAdvertisement
Hide AdProfessor Nicola Stonehouse, specialist in molecular virology at the University of Leeds, said: “People who are seriously ill with Covid-19 have around a 20 per cent chance of a blood clot.
“In contrast, we are looking at fewer than 100 people over the 20 million vaccinated with the Oxford/AstraZeneca vaccine.
“Therefore, the number of people affected is very, very small. And the benefits of vaccination still outweigh any risks.
“As more and more people are vaccinated, the data regarding which vaccine is better for whom comes to light.
Advertisement
Hide AdAdvertisement
Hide Ad“Note that in the early days of the Pfizer/BioNTech vaccine there were a small number of people who suffered a serious allergic reaction (anaphylaxis). This was attributed to a PEG allergy – and people with such allergies were advised to take the Oxford/AstraZeneca vaccine.
“Now we see that for some groups of people, e.g with a history of blood clots, that the Pizer vaccine may be better. As we now have three approved vaccines, and hopefully others on the way, these can be targeted accordingly.”